Many inspirational quotes for success and failure say success is personal, not the outcome, and failure isn’t the end… but in the medical world, I beg to differ. Success is a good outcome, and failure can mean harm or death. I think we all have ‘what if’ thoughts, and here, in a remote, low-resource medical setting, it’s often difficult to not ruminate on the failures, as they feel like your fault.
As Jonathan and I are doing a paracentesis in one room, a twin is born in the outhouse. The other nurses and aides situate mother and baby in our delivery room and encourage her to push. When I get there, I see the second twin’s placenta has come out before the baby…how long? Time to get this little one out. But mom seems stalled with pushing and the baby is high, albeit with head presenting. I find a vac-assist device and start pulling, worried this mom will have to go down for C-section if we don’t get the babe out. After a few good pulls, mom pushes, and a little blue girl is there. Not much sign of life. An occasional heartbeat. The rest of the staff encourage me to start CPR, which I do. Not much improvement, and I think of how hard life is for babies here, never mind tiny preemie twins, and a possible hypoxic brain injury? I talk to the mom. I tell her she has a beautiful girl, and she should name her and her sister. She can always tell her little girl she has a sister in Heaven. Surprisingly, the mom comes up with two names, Mirlandy and Mirlandia, and specifies which is for which. She is calm as she leaves.
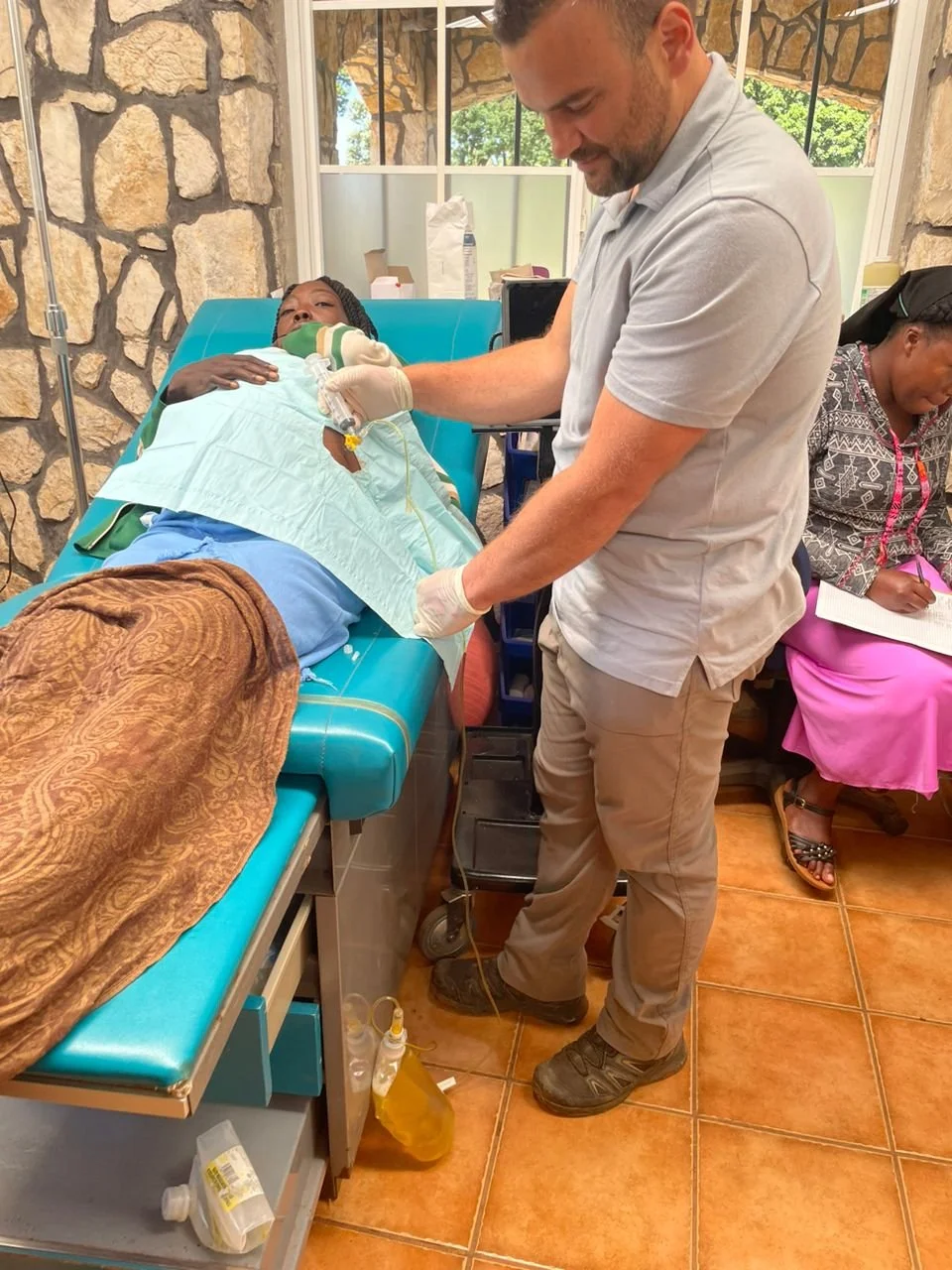
The paracentesis: liver failure, ascites, jaundice from? hepatitis? in a young lady. Came to us twice and we took off 6 liters each time before they went to Fond Parisien. FP hospitals said they couldn’t help; she needed a bigger hospital. So when they came back and asked us for help getting her past the gangs to one, we managed to get Haiti Air Ambulance to fly up. It was lovely to see Larissa again. And know that our patient would be getting the care she needed at last.
P.S. Word on the street 6 days later is that she died. Likely only a transplant would have saved her. What ifs crowd into my thoughts.
One of the youth boys came in with a 4-day foreign body in his eye from grinding metal. I did my best to remove it, first with a swab, then a plastic wand, and, finally, a needle tip (yes, this stuff is scary, but can be effective). Sadly, the little speck of metal had started getting embedded into the eye and I only got a piece off. Some research later, I found that the eye clinic in Roche Blanche was operating, open Monday to Friday, as per their website that had the date of 2023 on it, and I told him to rush down there (past the gangs) as fast as possible. Off he went.
The next day I had another eye injury come in. Well, I thought I knew where to refer. Tried to pull up the website again and what also came up was a letter saying that they were closed due to gang activity since November, not to refer patients there, etc. I was horrified. I immediately called the youth boy. No answer. Asked his family. Yup, he went down right away yesterday, and we haven’t heard from him since. Oh, one of the nurses said, yeah, that area is full of gangs. What had I done? Had I unwittingly sent him to his death?
A few long hours later my phone rings; the youth boy calling me back. I’m so sorry, I blurt out. I thought they were open and here I sent you into gang territory. No problem, he said. They were open. Took out the foreign body. Gave him a follow up appointment. Everything went well. Whewwwwwwwwwwww!!
We changed up our system here a bit, and it is more streamlined. With the central pharmacy, we now have the aides doing weights, vitals, etc. This frees up the nurses for more time with each patient, and more efficiently spent time. The results were immediately noticeable. The other day there were about 100 patients, and with 2 nurses we were done by 230. Pretty amazing. Our receptionist feels the pressure, though, and says he doesn’t have as much downtime now.
In my prenatal class I am adamant that they should not drink ginger tea in pregnancy, especially in the third trimester. I repeat, cajole, reiterate, make them repeat back to me, show pictures, hand out pamphlets, act out problems graphically, to what avail? A young girl comes to us. First baby, cramping. The nurses check her. Not dilated. The next day, again. I take one look. Ginger tea? Yes. And she has attended my class. 3 cm dilated. Later in the evening, the family has been to Forèt clinic (which has a real doctor) and sent home, and they are back. 4 cm. We can’t help this, it’s the ginger tea. By this time, they say they want to go to Fond Parisien. Sure. If we get a driver and they can pay the ambulance fee, do they want to go? Oh, no, they aren’t ready. Next afternoon they are wanting an ambulance ride but through all the back and forth with multiple people and discussing the price, we eventually don’t hear from them again.
A sister in the church gives birth on Friday, but I only hear about it Sunday afternoon when they come with the baby (mom still at home for the obligatory 14+ days) and say it isn’t breathing well. Looks like a baby boy peacefully sleeping, no nostril flaring, no respiratory distress. But when they went for further assessment to Jonathan’s, they say the baby hasn’t had any milk at all since birth, as he won’t breastfeed. What? This mom has raised 6 other children; how does she not think nourishment is important? And she came to prenatal class too, at least once. I talk A LOT about breastfeeding and formula preparation there.
Maybe I’ll have to stand on my head next prenatal class. Note to self: practice handstands. Or maybe someone who already knows how to do handstands wants to come in my place. I plan to leave for Canada in November, to put my Prenatal Class knowledge to practical use. The Board says I can leave if I find a replacement. So help me out here! Haha. -Nurse Carmina