I have not found a place where life and death, survival and ‘thrival’ hang so precariously in the balance as in this country of Haiti, and this last week has been no exception. The closure of the border by the Dominican president over a group of Haitian farmers trying to irrigate their drought-plagued land has affected everyone. Commerce is grinding to a halt on certain items, among those medication, fertilizer, and food. Banking and travel are going to be severely limited if not almost impossible, as the road to Port au Prince is hot with gang activity. What do we do? There are still blessings: gardens are being planted, rains are plentiful, cisterns are full at the moment.
The clinic numbers seemed to have leveled out and we see around 60 to 100 people a day. I had a lady who hadn’t been to the clinic since 2016, according to her chart. Her nonsensical explanation to this was that she heard the ‘whites’ were back, so here she was.
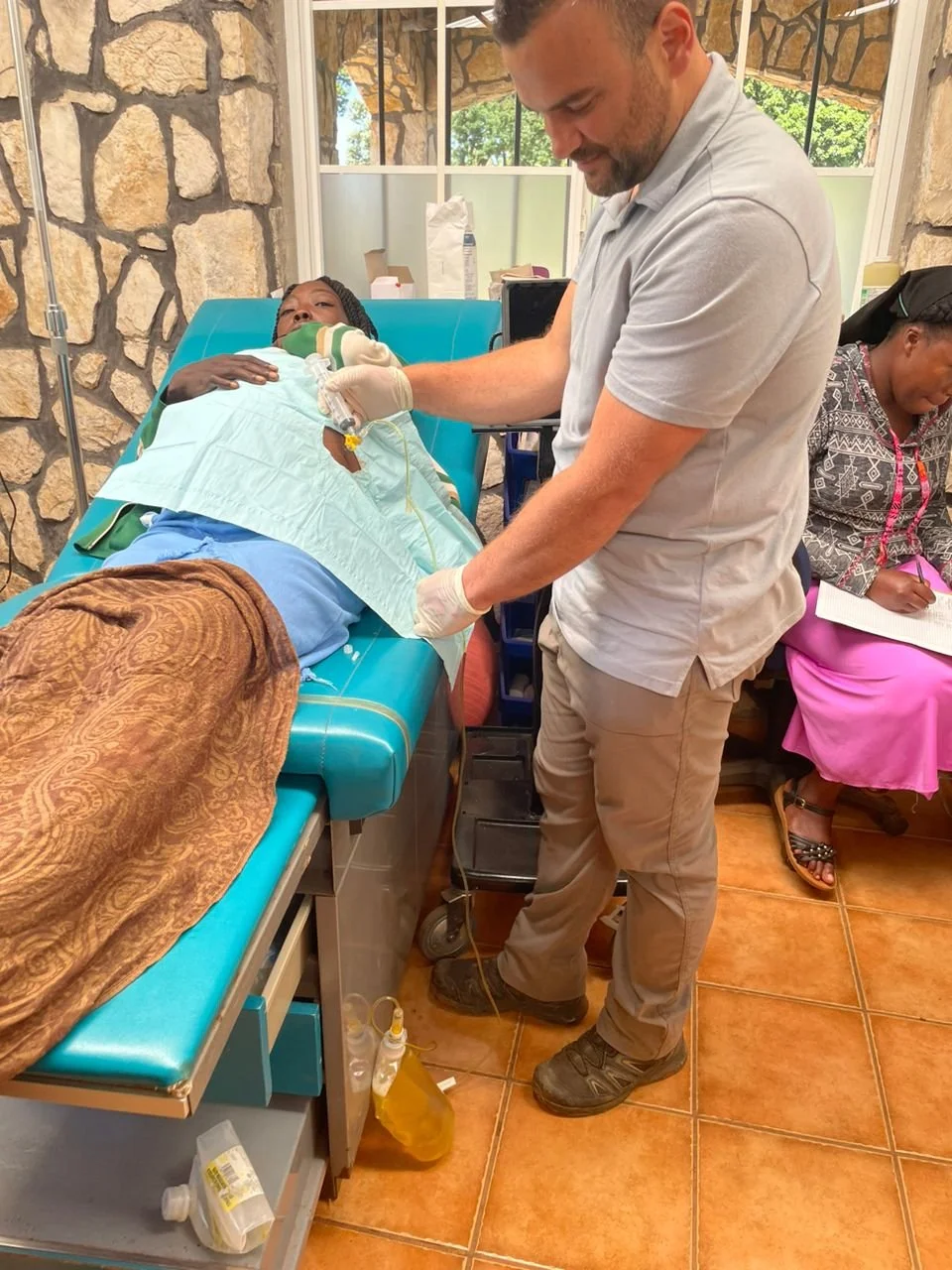
A lady gets carried up on a bed. The husband seems frantic, telling me she’s not talking, not eating, not drinking for three days. Others inform me that no, she has been getting nourishment. She says words to us. I dig deeper… only three days? She looks a lot sicker than that. Ok, about 9 days, with the last three being much worse. Ok… I ask what the leaf doctor gave her, tricking them into admitting they tried him first. A pill and a syrup, they tell me. Then he tells me they come from far away, and everyone listening bursts out laughing as he says Oplimèt, the area right next to Oriani and not considered far at all. Jonathan establishes an IV with the help of ultrasound, as her veins are pretty flat. Blood test shows HIV. I test the husband, who also has a non-healing dermatological condition on his chest. HIV positive. We explain the malady and put them in touch with the Croix-des-Bouquets TB and HIV clinic for the much-needed anti-retrovirals. It may be too late for the lady.
A mom silently labours as she waits for her prenatal consult and delivers almost as soon as she’s called into the consultation room. The quietest Haitian labor I’ve witnessed, I think! She doesn’t have a name picked out for her girl, so when Nurse Vitanie fills out the certificate we start suggesting. The mom rejects one suggestion of Roselande but takes my suggestion of Daphlinka (my go-to for naming baby girls here). I tell the mom she can give her two names, and suggest her name, Jackline, for the middle name. Mom seems quite enthused. Another bonus: she’s sitting on a hard bench, breastfeeding the minutes-old newborn as we discuss this. I have high hopes for this baby!
I am seeing a patient in my room when Sè Papi comes in with a bundle. Look at this baby, she says. A tiny baby, dead of malnutrition. We ask the mom when she had died. While she was waiting for her appointment here today she says. Yes she had gone to Forèt clinic with her. They said she was malnourished. Did she give the baby any milk or breastfeed her? No. She was a month old. The mom has a very flat affect and quite a few children at home. I add a piece about postpartum depression into my prenatal course.
Vitamin Angels donated prenatal meds, vitamin A, and albendazole, so we are working on rolling out a program where we try to keep better track of dewormer and supplements for children under 5 and continue pushing prenatal vitamins on all pregnant and breastfeeding moms. One old wives’ fable I’m trying to quench (one of the many!) is that taking prenatal vitamins will make your baby big and therefore make labour more painful.
MSPP, the national health care authority, has sent a vaccine nurse to help us for 6 months. Wednesdays are her busiest days, so in the meantime she helps out in the consult rooms and the pharmacy.
And coming up in November, the Lord willing, there will be a vacant position for a nurse. However, with the indeterminate DR border closure, will there even be enough supplies and funds to run a clinic at that time? This is a day-by-day adventure like none other, this Oriani clinic life! Please pray for us and the people we are here to help. We don’t know the future, but we know Who holds the future.