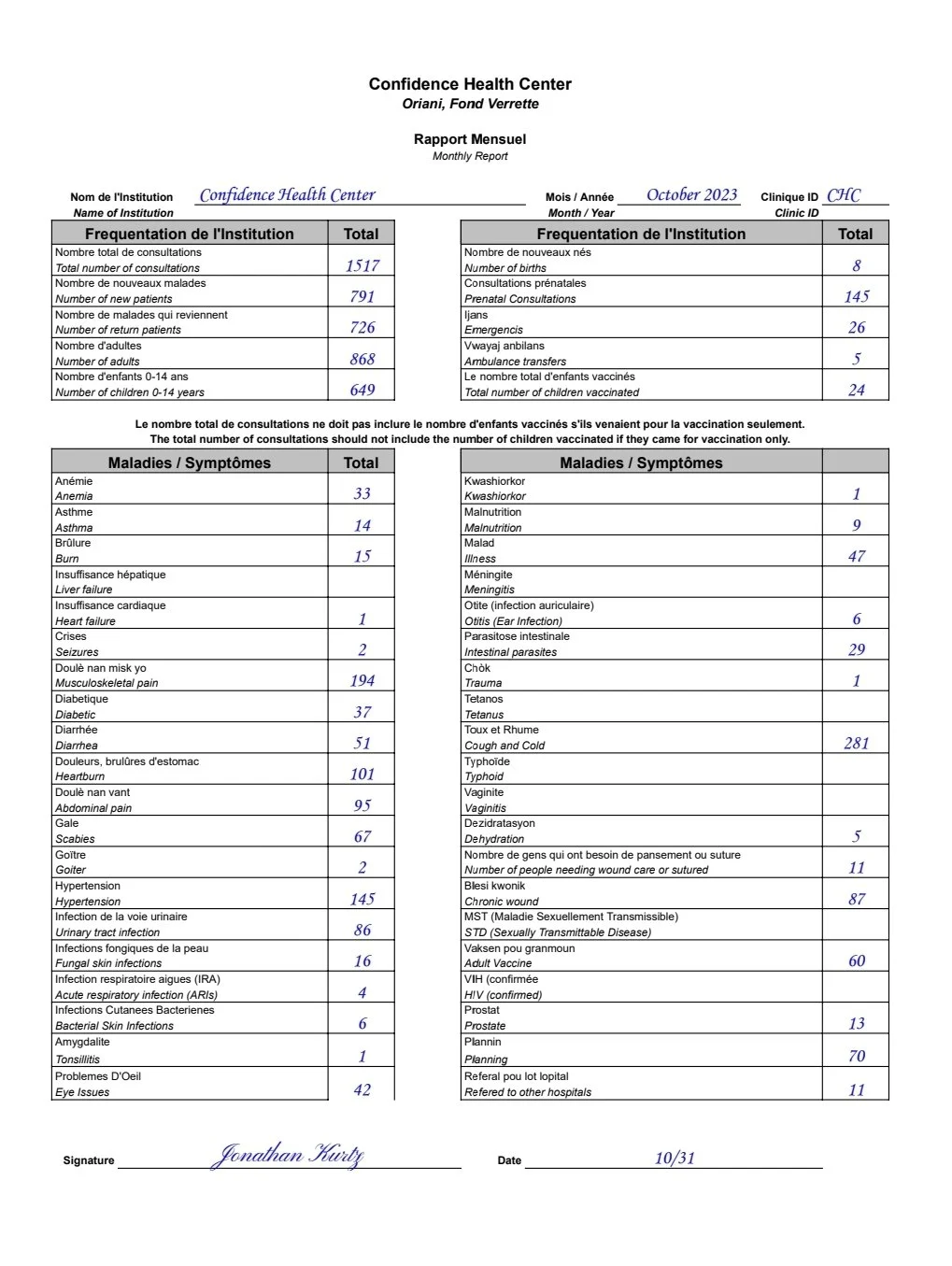
Hello to everyone from Oriani. As you can see from the report, November was a less busy month than October. While 1,100 patients is less than 1,500, it was still enough to keep us busy. A big change came when Carmina left at the beginning of the month. She helped me a lot in getting the clinic running, helping our nurses adapt to our way of doing things, revamping our protocols, and helping me learn to operate here. She is missed but we wish her well.
This will be a shorter than usual update as I am tired. I was up most of the night with a delivery. The delivery went well for the mom, but the placenta separated early and was delivered with the baby. The baby wasn’t breathing. I suctioned the nose and mouth thoroughly then started assisting breathing with a Bag Valve Mask (BVM). After about 10 minutes, when I had almost given up, the baby finally started breathing on her own. When they left the baby was opening her eyes and crying. After that long I am very concerned for an anoxic brain injury. God only knows how she will turn out.
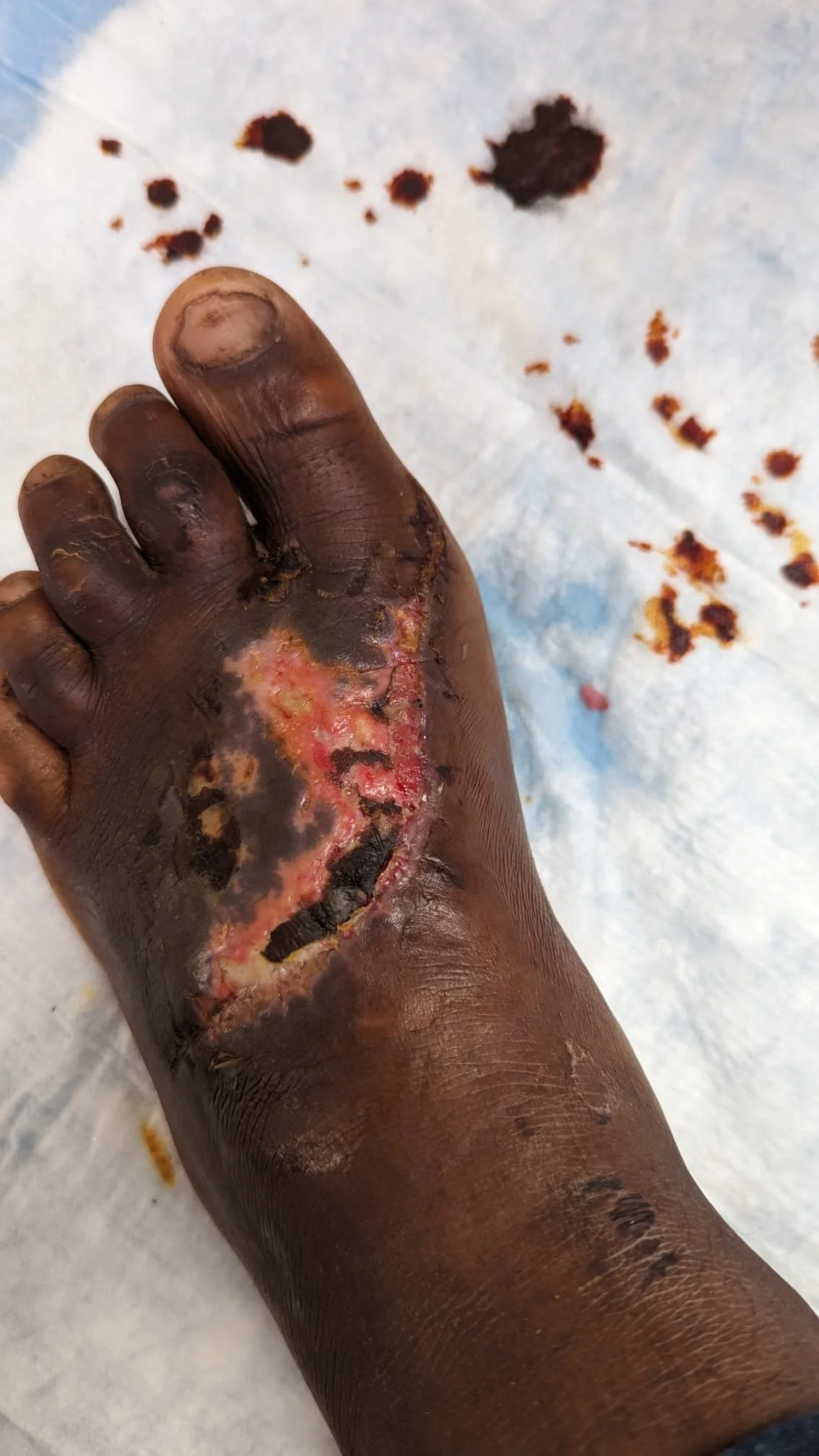
On the 13th a 15 year old boy was brought to our house after falling off a moto. He had a large wound on his left foot. At first I didn’t think I could close it enough to suture it. But after cleaning the wound, I was able to use X sutures to pull it together enough to suture the rest. After bending over his foot for an hour, my back seemed to be hurting me more than his foot was hurting him. I had numbed it with lidocaine, but he never flinched. I asked him several times if it was hurting him and he said no. I gave him Bactrim for antibiotic prophylaxis and a tetanus booster. He came back on the 16th and 20th for check ups and dressing changes. On the 1st we were able to remove his sutures and it seems to be healing well.
After placing several large orders of medications over the last 2 months, I can finally say the clinic is stocked with medications for 6 months. This has been my goal and going forward I will try to keep it stocked at that level. I want to thank everyone for your donations. Money donations are very important to allow us to buy supplies and pay our staff, but material donations are great too. We have received donated supplies from people in the US and Canada. Thank you for this. These are useful and often are things that we can’t buy here. We plan on going home for Christmas since the border seems to be opening. The clinic will be closed between Christmas and New Years to give our nurses the chance to go visit their families in Port au Prince. Thank you again for your support!